Autoimmune Series: Inflammatory Bowel Disease Effects on Oral Health
A group of Autoimmune diseases called Inflammatory Bowel Disease (IBD) results in chronic inflammation in the gastrointestinal (GI) tract. The two main diseases identified in this group are Crohn’s Disease and Ulcerative Colitis. The symptoms of chronic inflammation over time damage the GI tract. This can cause discomfort and painful symptoms for those affected.
The two diseases share many similarities and must be diagnosed by a physician. Crohn’s disease can take place anywhere along the GI tract, from the mouth to the anus. The small intestine is the most commonly affected area. The affected areas show up as patches of irritation next to healthy tissue and the inflammation may reach through multiple wall layers within the intestine. Contrarily, Ulcerative Colitis is localized to the colon and rectum. Different from the patchy areas seen in Crohn’s, the damaged areas in Colitis are seen in a continuous pattern, typically moving upward from the rectum to the colon. Colitis is also only found in the innermost wall of the colon as opposed to affecting multiple layers.
It is difficult to pinpoint the exact causes of Inflammatory Bowel Disease just like most autoimmune diseases. Research points to environmental and genetic factors as the likely source. The result is an immune response that when triggered by environmental factors attacks the cells in the GI tract. Both the Inflammatory Bowel Disease; Crohn’s and Colitis, share similar symptoms and can be easily misdiagnosed.
Symptoms Include:
-Persistent diarrhea
-Abdominal pain
-Rectal bleeding/bloody stools
-Weight loss
-Fatigue
IBD is different from IBS and Celiac disease. Getting the correct diagnosis is imperative for the best treatment. Unfortunately, because the symptoms are so similar it is common to be misdiagnosed. That is why it’s important to see a physician or IBD specialist.
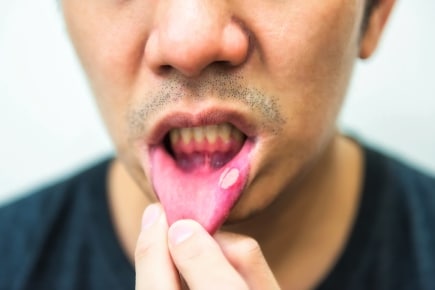
-Xerostomia (Dry Mouth): The salivary glands don’t produce enough saliva to keep the mouth moist and the pH of the oral cavity balanced. This can result in rampant decay.
-Aphthous Ulcers: Also known as canker sores. Individuals with IBD may present with frequent or multiple ulcers. These lesions can make oral care more uncomfortable.
–Mucosal Tags: Similar to skin tags, these can be seen as a result of Crohn’s Disease. They may appear on the inner cheek and can be visualized by your dentist or hygienist.
-Gingivitis: Reversible form of periodontal disease, is treated with good home care and professional hygiene visits.
If you are suffering from any of these oral symptoms we can help! Our doctor and hygienist will tailor a treatment plan that best suits your needs. For example, if you’re experiencing frequent aphthous ulcers you may be prescribed a steroid cream to decrease length and frequency. Or if you suffer from xerostomia, we’ll discuss options to balance pH and decrease your risk for decay. Having good home care and regular hygiene visits will help decrease any oral symptoms caused by the immune response. If you would like to discuss the impact your Inflammatory Bowel Disease may be having on your oral health, please feel free to mention it at your next visit!
References
